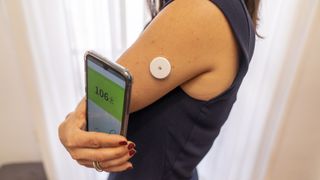
If you have Type 1 diabetes, a continuous glucose monitor (CGM) could help you better understand how exercise and food, among other factors, affect your blood sugar levels. While some people favor using one of the best glucose meters, a CGM is worth considering for anyone who tends to have blood sugar levels that frequently fluctuate. But how do continuous glucose monitors work, are they painful, and who should use them?
Studies have shown that 24/7 glucose monitoring can help reduce the risk of hypoglycemia and hyperglycemia, improving the quality of life for a wide range of patients. So if you’re looking for additional peace of mind, a CGM is worth considering.
Unfamiliar with this type of device and wondering if it’s right for you? No worries. In this article you'll learn how a continuous glucose monitor works, the pros and cons of CGMs, and how to use a monitor for accurate readings.
What is continuous glucose monitoring?
Continuous glucose monitoring automatically monitors your blood sugar levels 24/7, and a CGM is the wearable sensor that does the monitoring. CGMs are compact medical systems that enable people to monitor their blood sugar levels and get accurate readings in real-time. Most of them also show you readings over a series of hours, so you can better spot any emerging patterns.
There are only four FDA-approved CGM systems on the market right now, and two of them require no fingerstick calibration. While they aren't covered by the best Medicare Part D plans, CGMs made by Abbot, Dexcom and Senseonics are all covered by Medicare Part B. That's because they are classed as Durable Medical Equipment. The CGM manufactured by Medtronic is not currently covered by Medicare.
These devices are more expensive than traditional finger-prick devices and vary in price. Without coverage, a CGM can cost anywhere from $300 to $1,400, so speak to your health insurance company to see if you're covered. The sensors, most of which need to be changed every seven to 14 days, retail for between $40-$60 each.

How do continuous glucose monitors work?
Unlike a meter that requires you to prick your fingertips as many as seven to ten times a day, a CGM utilizes a small sensor wire that you insert just below the surface of the skin in your abdomen or the back of your arm. An adhesive patch holds the sensor in place where it takes glucose readings from the interstitial fluid (ISF) that surrounds the cells of the tissues beneath your skin.
Once the sensor takes a reading, usually once every five minutes, it's then transmitted to a handheld electronic device known as a reader. Sensors can usually be worn for seven to 14 days. However, the sensors on the new Eversense CGM from Senseonics have a wear time of 90 days, which is far more convenient.
What do CGMs consist of?
A continuous glucose monitor consists of a sensor, a transmitter and a receiver, so it's important to learn how they work and how to use them. There are differences between the various brands and models, so we recommend you always follow the manufacturer's instructions and consult your doctor if you’re unsure. Here’s how each of the three parts work:
- The sensor - consisting of a very thin wire that gets inserted under your skin with the aid of a needle, sensors are normally worn on the abdomen or back of the arm. Once the sensor has been inserted, it's secured with an adhesive patch to ensure it doesn’t move around. The sensor will detect glucose in the fluid between your cells, then sends its results to the transmitter.
- The transmitter - this is attached to the top of the area where the sensor is inserted. Once there it wirelessly sends information from the sensor to the receiver. You can buy a rechargeable transmitter or a non-rechargeable one that will need changing every few months.
- The receiver - (also known as the monitor) is a small handheld device with a screen where you’ll find all the data from your sensor displayed. You can also access past readings here. If you have a smartphone, you don’t need a handheld device and can instead get all the information via your chosen CGM's app. The receiver will send you a warning in the form of an alarm if your blood sugar level is either too high or too low.
Do continuous glucose monitors hurt, and are they easy to use?
A CGM can take a bit of getting used to, but once you’ve got the hang of it, these devices are simple, straightforward and pain-free. You’ll need to spend a bit of time initially getting up to speed with how your CGM works, which includes:
- Learning how to insert the sensor correctly (full instructions will be included).
- Whether it requires calibration with fingerstick blood glucose readings (some don’t).
- How to set the alarms to receive alerts when your blood sugar is too high or too low.
- How to transfer and store your readings safely for long-term analysis.
Think of your new monitor in much the same way as any new piece of technology - it can take a few days to get used to a new setup, but once you do, a CGM offers additional peace of mind when paired with a traditional meter.

Who should use one?
Most people who currently use CGM’s have Type 1 diabetes. However, researchers are looking into how these devices may help the more than 30 million Americans with Type 2 diabetes, and the 84 million who have pre-diabetes. The National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) notes that a CGM may also be recommended to adults and children who:
- Are on intensive insulin therapy
- Have hypoglycemia unawareness
- Often have high or low blood glucose
While a blood meter reader is an effective way of monitoring glucose levels, a CGM is a great complementary tool that can help you better understand how physical activity and food can affect your glucose levels throughout the day and night.
The advantages of using a CGM
Since CGM’s continually collect readings, the biggest advantage to using one is that they provide you with real-time information on what’s happening with your blood glucose. This means you should be able to identify issues immediately. The fact tht you can store readings over a period of time can also help your health care professional when it comes to adjusting your treatment plan.
There’s also the advantage of having fewer fingersticks to contend with, and a CGM can help to reduce the likelihood that you’ll suffer from a low blood glucose emergency.
The drawbacks of using a CGM
Depending on the level of insurance cover you have, one of the major drawbacks is the upfront and ongoing costs associated with a CGM. Until they more widely available, and there are a greater number of devices to choose from (which will help lower the prices), some people might be priced-out of owning one of these devices.
Insertion of the sensor may be a turnoff for some people, and it’s possible to experience skin reactions over time with the adhesive that’s used to attach the sensor to the skin.
You also can’t yet rely on a CGM alone. While researchers are working to make these devices easier to use and more accurate, you’ll still need to do a finger-stick glucose test at least twice a day to ensure your insulin dose is correct.
Unsure whether a CGM is right for you at this time? Then here are some popular traditional glucose readers to check out...